Introduction
This course will teach you about first heart sound auscultation. Before beginning this course, you should have finished the Normal Heart Sounds course and feel comfortable with your ability to listen and recognize normal heart sounds and to be able to identify the first heart sound.
- Understand S1 sound components
- Identify S1 wide splitting
- Differentiate S1 from S2
Overview
When the mitral and tricuspid valves close, vibrations in the heart are transmitted to the chest wall as the first heart sound ('lub'). The first heart sound (S1) will occur immediately before the patient's pulse is felt at normal heart rates. S1 is usually heard immediately after the QRS complex. Splitting is common in children and is about half of normal adults.
In normal cases, the mitral and tricuspid valves close within 20-milliseconds of each other. Thus, the first heart sound is heard as a single sound. However, certain heart conditions can delay the tricuspid closure, widening the mitral - tricuspid valve opening gap, resulting in a split first heart sound.
M1 is best auscultated at the apex, using the diaphragm pressed firmly to the chest wall. T1, the second component of S1, may be heard at the left lateral sternal border (LLSB), using the diaphragm. In some first heart sound splits, M1 and T1 may not be separately heard, rather S1 is heard as a 'slurred' sound. S1 splits are not affected by respiration.
Intensity
The mitral component (M1) will be best heard at the apex. The tricuspid component (T1) is best heard at the LLSB. Sound intensity will be loudest with thin chest wall. Strong ventricular contractions (e.g. with exercise) contribute to higher intensity. A short EKG PR interval also increases loudness.
Widely Split S1
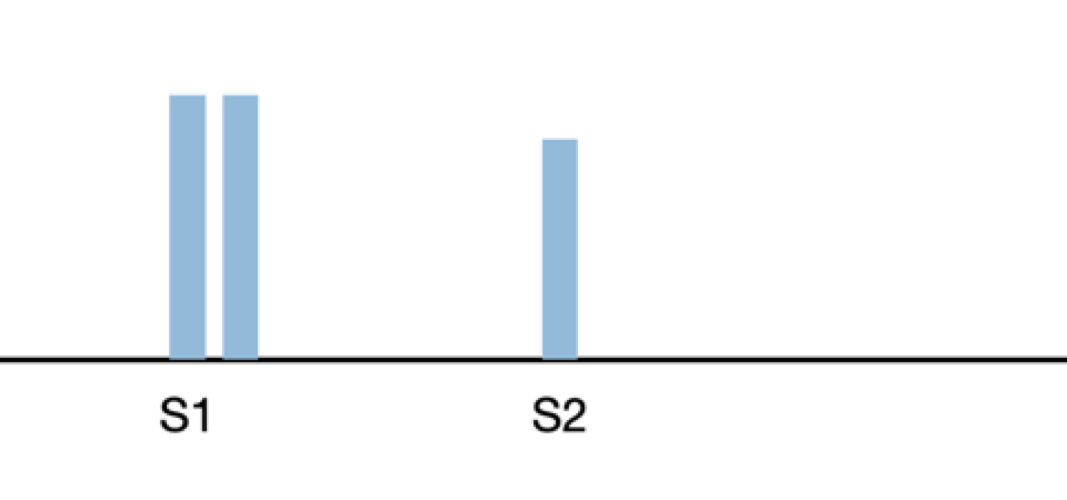
Widely split S1 is caused by delayed right ventricle contraction. This split can be associated with right bundle branch block, atrial septal defect, ventricular tachycardia and Epstein's anomaly.
Identifying S1 from S2
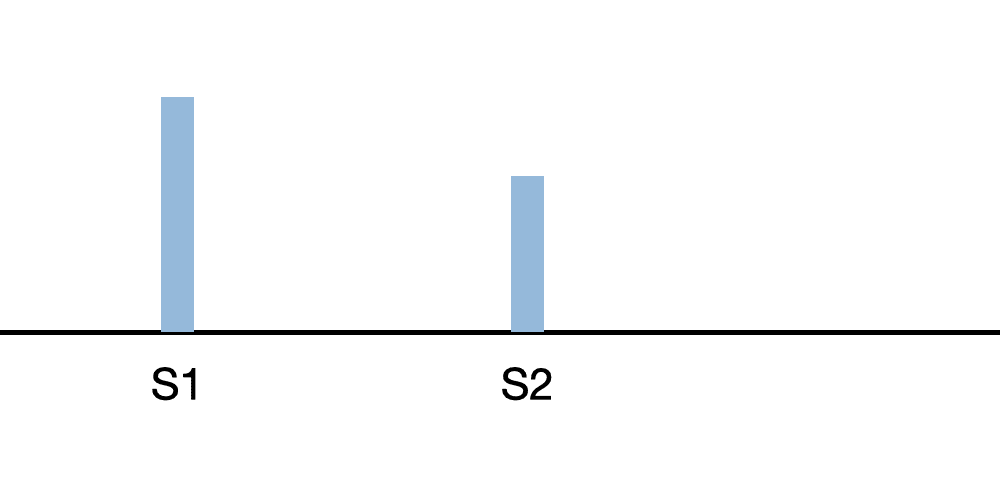
At heart rates below 80 BPM, S1 follows the longer pause. At higher heart rates, the diastolic interval will be shorter and approximately equal to the systolic interval.
In normal patients, S2 will be loudest at the base. S1 will be louder at the apex compared to other auscultatory sites.
Another technique is to palpate the carotid pulse while auscultating. S1 occurs slightly before the carotid pulse is felt.
Start First Heart Sounds Course
First Heart Sounds Lessons
Loud First Heart Sounds
This heart sound lesson is also found in the 'Normal Heart Sounds' module.
The first heart sound is usually slightly louder than the second when auscultating at the mitral valve (apex).
The first heart sound is much louder than the second heart sound in this case. A thickened but still movable mitral valve is generating this particular sound. Look at the anatomy video to see the thickened mitral valve leaflets.
Loud first heart sounds can also be observed in patients with thin chests.
Minimally Split First Heart Sound
This heart sound lesson is also found in the Normal Heart Sounds module.
Commonly, the first heart sound consists of two sounds separated by a very small interval (20-30 milliseconds). The mitral sound (M1) typically occurs before the tricuspid sound (T1). T1 and S1 splitting can be best heard at the tricuspid location. If M1 and T1 are separately distinguished, this is called an S1 split. S1 splitting is common in children. An S1 split can be associated with EKG-related abnormalities such as right bundle branch block, premature ventricular contractions, or ventricular tachycardia in adults.
A minimally split first heart sound is a normal variation of the first heart sound.
Minimally Split First Heart Sound Lesson
Markedly Split First Heart Sound
Splitting of the first heart sound is audible when the split interval is 50 milliseconds or higher. Auscultation is best performed at the tricuspid area to observe such splitting sounds. When the chestpiece is shifted to the apex, the mitral component of the split heart sound becomes louder. Markedly split first heart sounds is an auscultatory indication of premature ventricular contractions or right bundle branch block
Markedly Split First Heart Sound Lesson
Decreased Intensity First Heart Sound
Abnormalities, such as a previous heart attack, decreased thyroid function, congestive heart failure, coronary artery disease, AV Blocks, cardiomyopathy, and mitral regurgitation. The anatomy video provides one example of such conditions.
In addition, thick chest walls can dampen the transmission of heart sounds, resulting in the observation of diminished heart sounds
Decreased Intensity First Heart Sound Lesson
Fourth and First Heart Sounds
A fourth sound gallop (S4) plus a first heart sound (S1) can mimic a split first heart sound. Since the S4 occurs just before the S1, it is easy to confuse a S4-S1 pair with a split S1.
Listen carefully to the frequency of the initial sound of the S4-S1 pair. If it is lower in frequency than the second sound, it is an S4. If the two sounds have a similar frequency, it is a split S1.
Fourth and First Heart Sounds Lesson
First Heart Sound with Aortic Ejection Click
An aortic ejection click is produced by thickened aortic valve leaflets. These clicks can be generated in a bicuspid aortic valve, which is a congenital abnormality with two aortic valve leaflets instead of the three normal leaflets.
A single first heart sound (S1) followed by an aortic ejection click (AEC) can mimic a split first heart sound. An AEC follows S1 by 50 milliseconds. An AEC will have a higher pitch and shorter duration than S1. The recommended auscultation point is the aortic valve area where splitting of S1 is not heard.
First Heart Sound with Aortic Ejection Click Lesson
Course Quiz
After completing all lessons in a course, a quiz becomes available. If the user successfully completes a quiz, results are saved to the user's dashboard and a certificate can be printed.
Reference Guide
For subscribers, we provide a comprehensive heart sounds and murmurs reference guide. For each abnormality, one or more sound recordings are available along with text, phonocardiogram and cardiac animation.Course Completion
Registered users can earn a certificate of achievement for this module by reading all content and then earning a passing score on this module's quiz.
Completed modules and related scores can be viewed on the dashboard.
Authors and Reviewers
-
Heart sounds by Dr. Jonathan Keroes, MD and David Lieberman, Developer, Virtual Cardiac Patient.
- Reviewed by Dr. Barbara Erickson, PhD, RN, CCRN.
-
Last Update: 11/9/2021
Sources
-
Heart Sounds and Murmurs Across the Lifespan (with CD)
Dr Barbara Ann Erickson
Publisher: Mosby
ISBN-10: 0323020453; ISBN-13: 978-0323020459 -
Heart Sounds and Murmurs: A Practical Guide with Audio CD-ROM 3rd Edition
Elsevier-Health Sciences Division
Barbara A. Erickson, PhD, RN, CCRN - How to measure blood pressure using a manual monitor
Mayo Foundation for Medical Education and Research (MFMER) -
Heart and Lung Sounds Reference Guide
PracticalClinicalSkills.com -
Manual Blood Pressure Measurement
Vital Sign Measurement Across the Lifespan