The Stethoscope
1. Auscultate the patient in a quiet and well-lit room. Ambient noise should be minimized as much as possible by closing doors and briefly not talking with the patient.
2. The patient can be examined in three positions: sitting, supine, and left lateral recumbent. In our heart and lung sound lessons, we will indicate the patient’s position.
3. Place the stethoscope chestpiece in direct contact with the chest wall.
4. Learn to use a stethoscope's bell and diaphragm. When using the bell, press lightly because this allows low-frequency sounds to be optimally heard. When using the diaphragm, firmer pressure aids in hearing higher-frequency sounds. Some stethoscopes have a chestpiece that performs as a bell or diaphragm by varying the chestpiece pressure on the chest wall.
Where to listen to heart sounds
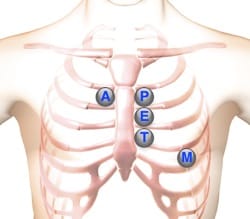
When listening for cardiac sounds, start with the stethoscope's diaphragm, and then use the bell, at each position. Try to establish a fixed sequence as you auscultate these areas: - Lower left sternal border (4 ICS) for tricuspid valve and right-heart sounds - Apex (5 ICS in mid-clavicular line) for mitral valve or left heart sounds. - Aortic (2 ICS) for aortic valve sounds - Pulmonic (2 ICS) to the left of the sternum for pulmonic valve sounds - Erb’s Point (2 ICS) to the left of the sternum.
 |
Aortic Valve Area | Second right intercostal space (ICS), right sternal border | |
 |
Pulmonic Valve Area | Second left intercostal space (ICS), left sternal border | |
 |
Erb's Point | Third left ICS, left sternal border | |
 |
Tricuspid Valve Area | Fourth left ICS, left sternal border | |
 |
Mitral Valve Area | Fifth ICS, left mid-clavicular line |
How to Listen to Heart Sounds
This website has over 100 heart and lung sound lessons. Within each lesson the author has indicated the point of auscultation. Use these links to learn more:
Other Physical Exam Components
A cardiovascular physical examination includes several components, with auscultation being the focus of this web page. In addition to listening for heart and vascular sounds during auscultation, it's important to evaluate blood pressure levels and observe jugular venous pulse patterns while performing inspection, as well as palpate apparent anatomical features on the precordium.